Protecting NHS workers
Keeping lone working staff safe has long been a key consideration for the NHS, which has an estimated 400,000 lone workers operating across its services.
Six years ago the NHS published a report on lone worker safety, which recommended that NHS organisations not only prioritise protecting their lone working staff, they should also consider using apps to do so.
Since this report, we have seen a huge rise in NHS organisations opting to use a lone worker app to protect their staff, as the increase in smartphone use makes a lone worker app a cost effective and easy-to-use alternative to the devices of previous decades. They also address one of the biggest issues faced by NHS employers when it comes to lone worker safety; ensuring that staff are using the solution they are provided with, every day.
Here we take a look at how the lone worker safety landscape has evolved in the NHS since this seminal report was published and provide you with actionable insights into how you can better protect the lone working staff within your trust today.
Who is currently responsible for lone worker safety in the NHS?
NHS Protect – the organisation which supported and advised hospitals in England on staff safety – was disbanded in 2017. Staff safety is now the responsibility of NHS Trusts, who can make their own decisions on how to safeguard staff, including carrying out their own risk assessments and producing their own lone worker policies. Trusts can also decide which type of lone worker protection would be the most appropriate investment for their workforce.
As well as lone worker safety being the responsibility of individual trusts, the number of lone working staff in the NHS is also increasing. In 2015, approximately 30% of the total NHS workforce – 332,468 staff members – were lone workers.
Based on 2020 NHS staffing figures, it is estimated that this number will have risen to just under 400,000 lone workers currently operating across NHS England, which in turn has put additional pressure on trusts to prioritise their safety.
Is the level of risk to NHS lone workers increasing?
In early 2020, Health Secretary Matt Hancock addressed an open letter to NHS staff pledging to tackle increases in violence, following a survey in 2019 that found that 15% of NHS staff experienced physical violence from members of the public and patients in the past year. Results from the 2020 NHS staff survey reported similar numbers; amongst NHS staff who have frequent face-to-face contact with service users, more than one in three claim to
have experienced at least one incident of bullying, harassment or abuse in the past 12 months and 14.5% of staff experienced at least one incident of physical violence – with ambulance service staff most at risk.
The World Health Organisation (WHO) estimates that between 8% and 38% of health workers suffer physical violence at some point in their career with many more being threatened or exposed to verbal aggression. Most violence is perpetrated by patients and visitors, and those most at risk include nurses and other staff directly involved in patient care such as midwives, A&E staff and paramedics.
According to the latest figures from the HSE, violent and aggressive incidents are the third biggest cause of injuries reported under RIDDOR from the health and social care sector.
COVID-19 and social distancing measures have also had an impact on levels of violence in the workplace, with heightened stress levels and changes in working patterns leading to increased levels of aggression, as well as an increase in people working alone.
In response to the high levels of violence against NHS staff during the pandemic, the NHS, the Metropolitan Police Service (MPS) and Crown Prosecution Service (CPS) have launched Operation Cavell across London, which aims to increase convictions and protect frontline NHS staff from violence.
“Over the past three months alone NHS and LAS (Locum Appointment Service) colleagues have been punched, kicked, spat at, urinated on, strangled, thrown across a room, had faeces thrown on them and been racially abused…Operation Cavell was launched to change this during a time when the NHS are facing pressures like never before” said Chief Inspector Luke Mooney from the MPS.
Digitisation within the NHS has helped to welcome lone worker apps
Whilst the need to protect NHS staff is clear, the Lone Worker Estate Mapping Exercise found it ‘surprising’ that more NHS employees didn’t use lone worker safety apps to do so, stating that they are cost effective and recommending that NHS organisations are made aware of their usefulness, especially as funding is often a key barrier.
In recent years, the NHS has become more open to the use of digital solutions; the NHS App Library – first launched in 2017 – features a host of digital health tools focusing on areas including mental health, sleep, diabetes and social care and NHS Digital also launched the NHS app in 2019, which can be used to book appointments and order prescriptions.
This trend towards app usage has also transferred into an increase in NHS organisations using apps to protect their lone workers. Several organisations such as Primary Integrated Community Services and Chelsea and Westminster NHS Trust are now using lone worker apps to protect their staff, in what is a growing trend in lone worker app usage across all sectors.
The benefits of apps for NHS lone workers
Apps are also able to better demonstrate a positive ROI – and increased protection of staff – because usage is visible and monitored.
The report came to the following conclusions;
“The most significant difficulty with lone worker systems is usage, with a great deal of effort put into trying to monitor and improve use of devices.”
“There is an issue with ownership of lone worker responsibilities and systems; this can be seen in the number of ‘unknown’ lone worker devices used by organisations.”
These two points are both addressed through the use of a lone worker app like StaySafe, which is used by multiple NHS Trusts and healthcare organisations to protect their staff.
As lone worker apps utilise cloud-based technology and sophisticated monitoring and reporting systems it is possible to see who is using – or not using – the app and follow up with specific team members to offer extra support. It is also easy to reallocate app licenses between team members to ensure that you are keeping track of costs.
“What we commonly see with customers who switch to an app is that they are looking for a way to track who is using the system. I’ve lost count of the amount of times I’ve heard employers say that lone worker devices like badges are being left at home or in offices, uncharged and unused. They switch to us because with our app, not only are employees already using their smartphones everyday, they get full visibility and peace of mind that every team member who should be protected, is protected” says Alan Coulter, Major Account Director at StaySafe.
The importance of ensuring employee engagement and usage of safety solutions is echoed by Kim Sunley, Senior Employment Relations Adviser, Royal College of Nursing:
“Many employers are saying the right things and have the right policies [around staff safety], but what is really needed is for those policies to be a reality in practice”.
Making staff safety a ‘reality in practice’ is something StaySafe have addressed through the development of our Customer Success Team, who work closely with every client to successfully on-board, train and provide on-going support to users of our lone worker safety app.
StaySafe clients have access to a range of dashboards and reports, allowing them to drill down into staff usage and address any areas of concern. The app also features in-app training, which all new users must complete, ensuring they are fully up to speed with how to use the app from the first time they log-in. If they have any subsequent issues or queries, our customer support team are on hand via webchat, phone or email to provide assistance.
Find out more about how StaySafe ensures high user engagement.
StaySafe and NHS lone worker safety
Since the Lone Worker Estate Mapping Exercise was published we have seen a steady increase in NHS organisations taking the reports findings on board and using a lone worker app to keep their staff protected whilst they work alone.
As part of the G-Cloud 12 Government Purchasing Framework for cloud based services, StaySafe provides NHS organisations with a cost-effective solution which is easy to use and deploy.
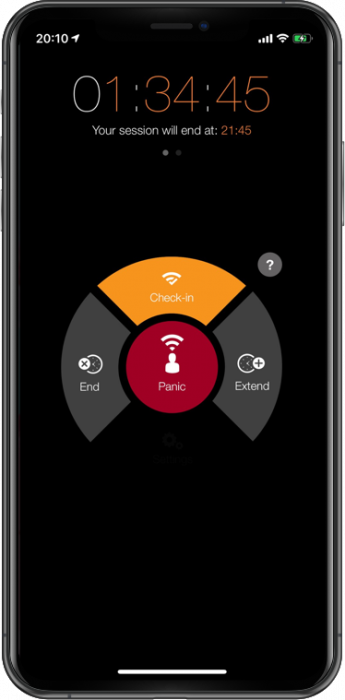
The StaySafe app gives NHS organisations visibility of the location and safety status of lone working staff and allows them to check-in safely once they have finished a lone working or travel session – or signal for help at any time. The app can also be paired with a range of discrete panic alarms which can also be worn or carried by staff.
The app also provides 16% more signal coverage than any other app via our low signal mode, which comes as standard for all app users. When low signal mode is active, the app only needs a 2G connection to maintain communications with the monitoring hub. In addition, missed check-in alerts still signal in the Hub even if the employee has lost signal coverage completely.
Monitoring and escalation of alerts can be done in-house by the trust or at a team level, or outsourced to our 24/7 professional monitoring partners. Ensuring a smooth roll out and high usage levels of the app is also taken care of by our dedicated Customer Success Team.
Find out more about why companies choose StaySafe